The Viral Warning That Shook the K-Beauty Community
Recently, a post began circulating on the popular community platform Instiz that sent chills through tens of thousands of readers. Titled with a warning about side effects so severe they lead to ‘extreme choices,’ the post quickly garnered over 52,000 views and dozens of frantic comments. As an ingredient specialist and fact-checker here at SYNC SEOUL, I usually spend my time looking at serum formulations. However, the science of our bodies doesn’t stop at the skin’s surface. When a medical procedure often marketed alongside cosmetic rhinoplasty—known in Korea as ‘Functional Rhinoplasty’ or Gineung-ko—starts showing up in reports linked to severe psychological distress, it is time to break down the science behind the headlines.
The procedure in question is rhinitis surgery, specifically turbinoplasty or turbinectomy. For those suffering from chronic nasal congestion, it sounds like a miracle: a quick surgical fix to breathe clearly. But for a subset of patients, the result is a living nightmare known as Empty Nose Syndrome (ENS). This isn’t just a minor complication; it is a physiological disruption that alters the way the brain perceives life’s most basic function: breathing. Let’s look at what the research says about why this happens and why the K-beauty world needs to take a step back from the ‘easy fix’ narrative.
“I saw that post on Instiz last night and I couldn’t sleep. My brother just scheduled his turbinoplasty for next month. Is it really this dangerous? People are talking about it like it’s a death sentence for your mental health.” — Instiz User
Understanding the Anatomy: More Than Just a Tube
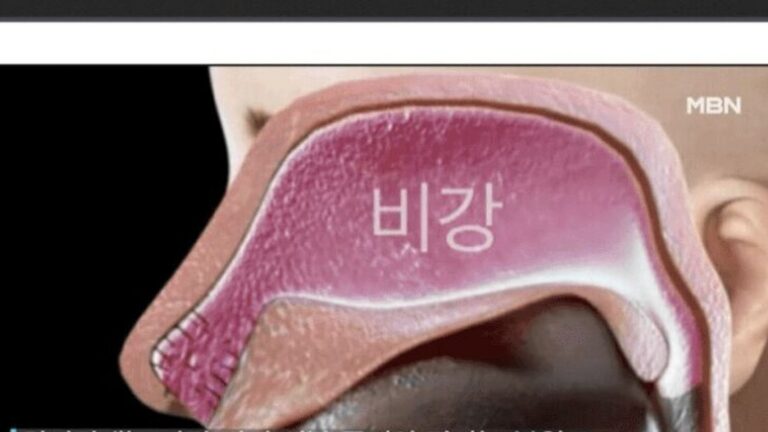
To understand what goes wrong, we have to understand what the nose actually does. Most people think of the nose as a simple pipe that carries air to the lungs. From a biological standpoint, it is far more complex. Inside your nasal cavity are three pairs of long, thin bones covered in a layer of tissue. These are called turbinates. Their job is to warm, humidify, and filter the air you breathe. They are the ‘air conditioners’ of the human body. Without them, the air hitting your lungs would be cold, dry, and irritating.
The inferior turbinate, the largest of the three, is usually the target of rhinitis surgery. When someone has chronic rhinitis, this tissue becomes permanently swollen, blocking airflow. Surgeons perform a turbinoplasty to shrink the tissue or a turbinectomy to remove part of the bone and tissue entirely. The goal is to create more space. However, the science is clear on this: space does not equal better breathing. If a surgeon removes too much tissue, the aerodynamic flow of the nose is destroyed. The air no longer spirals and warms; it rushes in like a cold draft in an empty hallway. This is the beginning of the ‘Empty Nose’ phenomenon.

A common misconception is that ‘more air’ is always better. In reality, the brain needs to feel the pressure and temperature of the air against the nasal mucosa to register that a breath has been taken. This is mediated by the trigeminal nerve. When too much turbinate tissue is removed, the sensors are gone. You might be moving massive amounts of air into your lungs, but your brain is screaming that you are suffocating. It is a terrifying form of sensory-neural mismatch that clinical studies have struggled to quantify because, on a standard CT scan, the nose looks ‘perfectly clear.’
The Science of Suffocation: Why ENS Leads to Extreme Outcomes
Why does the Instiz post mention ‘extreme choices’? To a healthy person, the idea that a clear nose could lead to such a dark place seems hyperbolic. But from a neurological standpoint, it makes perfect sense. Imagine the feeling of holding your breath for 60 seconds. That panic, that ‘air hunger,’ is what ENS patients feel 24 hours a day, 7 days a week. Because the brain doesn’t receive the signal that it’s breathing, the autonomic nervous system stays in a state of ‘fight or flight.’ This leads to profound insomnia, cognitive dysfunction (often called ‘brain fog’), and eventually, clinical depression.
Recent research indicated that the psychological burden of ENS is comparable to late-stage chronic obstructive pulmonary disease (COPD), yet patients often face ‘medical gaslighting.’ Because the physical obstruction is gone, many doctors tell patients their symptoms are ‘all in their head.’ This lack of validation, combined with the physical sensation of constant suffocation, creates a perfect storm for psychological collapse. The science of the ‘breathing reflex’ is so fundamental to our survival that when it is broken, the mind often follows.
“The worst part isn’t the physical pain; it’s the gaslighting. Every ENT I visit says my airway is ‘perfectly clear’ while I feel like I’m gasping for air in a vacuum. I haven’t slept more than two hours at a time in three years.” — Anonymous Sufferer, Support Group Comment
The K-Beauty Connection: The Rise of ‘Gineung-ko’
In the context of Seoul’s beauty industry, rhinitis surgery has seen a massive surge due to ‘Functional Rhinoplasty’ (기능코). This is a trend where patients combine a functional surgery (like septoplasty or turbinoplasty) with a cosmetic nose job. The lure is twofold: first, it’s efficient to go under anesthesia once for two goals; second, in Korea, the functional portion is often covered by private medical insurance, significantly lowering the overall cost of the cosmetic procedure. This financial incentive has led to an explosion of surgeries that might not have been strictly necessary.
From a formulation and safety standpoint, we always advocate for the ‘least invasive first’ approach. In the rush to get a slimmer, higher nose bridge through Gineung-ko, some clinics may be overly aggressive with the internal functional work. If a cosmetic surgeon who isn’t an expert in nasal physiology performs the turbinate reduction to make room for a silicone implant, the risk of ENS skyrockets. We are seeing more and more cases where young women and men go in for a ‘pretty nose’ and come out with a functional disability that destroys their quality of life.

The statistics are sobering. While the official incidence rate of ENS is claimed to be low, many experts believe it is vastly underreported because there is no standardized diagnostic tool. Most patients are only diagnosed after they have visited five or six different specialists. In a culture like Korea’s, where aesthetic perfection is highly valued, the shame of a ‘failed’ surgery—especially one that looks fine on the outside—prevents many from seeking the help they need until they are in a state of total crisis.
Fact-Checking the ‘Cure’: Can Empty Nose Syndrome Be Fixed?
If you or someone you know is suffering from these symptoms after a surgery, what does the science say about recovery? Unfortunately, there is no simple ‘undo’ button for a turbinectomy. Once the tissue is removed, it does not grow back. However, the medical field is evolving. Currently, we are seeing more success with ‘endonasal volume restoration.’ This involves injecting fillers or, more permanently, surgically placing implants (made of rib cartilage or synthetic materials like Medpor) into the nasal side walls to recreate the resistance that the turbinates once provided.
The goal of these treatments is to narrow the airway. It sounds counter-intuitive—why would you want a narrower airway?—but the science of fluid dynamics explains it. By narrowing the path, the air speed increases and the air is forced against the remaining sensors in the nose. Recent studies have shown that while this doesn’t ‘cure’ ENS, it can significantly reduce the sensation of air hunger and improve sleep quality. But let’s be clear: these revision surgeries are expensive, technically difficult, and not guaranteed to work.
“Functional rhinoplasty is the trend right now because of the insurance benefits, but seeing these side effects makes me want to cancel my consultation immediately. No aesthetic change is worth losing the ability to feel myself breathe.” — Beauty Community Member
Practical Advice: How to Protect Your Health
Before you agree to any nasal surgery, especially if it’s being bundled with a cosmetic procedure, you must be your own advocate. The science is clear that conservative management should always be the first line of defense. This includes long-term use of nasal steroid sprays, saline rinses, and identifying environmental allergens. Surgery should only be considered when all other options have failed and the quality of life is already severely impacted by the inability to breathe.
If you do proceed with surgery, ask your surgeon these specific questions: What technique are you using? Are you performing a total or partial turbinectomy? (Avoid total removal at all costs). How much of the inferior turbinate will remain? A surgeon who dismisses the risk of Empty Nose Syndrome as ‘a myth’ or ‘purely psychological’ is a surgeon you should walk away from. The most reputable ENT specialists are those who use ‘out-fracturing’ techniques or micro-debrider submucosal resections, which preserve the vital surface tissue and nerves while shrinking the underlying bulk.
The Verdict: A Warning to the SYNC SEOUL Community
The science of beauty is not just about what we put on our skin; it’s about the integrity of our biological systems. The viral post serves as a grim reminder that ‘routine’ surgeries carry life-altering risks. Rhinitis surgery is not a minor ‘tweak’ to be added to a cosmetic package for a discount. It is a high-stakes intervention in one of the body’s most sensitive sensory environments.
At SYNC SEOUL, we believe in informed consent. We believe that knowing the EWG rating of your moisturizer is important, but knowing the physiological risks of your surgery is vital. The ‘Empty Nose’ is a silent, invisible, and devastating condition. If the K-beauty industry is to remain a global leader in health and aesthetics, it must prioritize the ‘Skin-First, Health-First’ philosophy over the convenience of insurance-bundled procedures. Do not let the promise of a perfect profile rob you of your peace of mind. Your breath is your life—protect it fiercely.